Angina (an-JI-nuh or AN-juh-nuh) is chest pain or discomfort that occurs when
your heart muscle does not get enough blood. Angina may feel like pressure or a
squeezing pain in your chest. The pain may also occur in your shoulders, arms,
neck, jaw, or back. It may also feel like indigestion.
Angina is a symptom of coronary artery disease (CAD), the most common type of
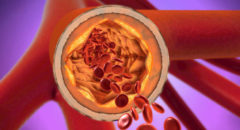
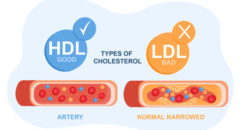
heart disease. CAD occurs when plaque builds up in the coronary arteries. This
buildup of plaque is called atherosclerosis. As plaque builds up, the coronary
arteries become narrow and stiff. Blood flow to the heart is reduced. This
decreases the oxygen supply to the heart muscle.
Types of Angina
The three types of angina are stable, unstable, and variant (Prinzmetal’s).
It is very important to know the differences among the types.
- Stable angina. Stable angina is the most common type. It occurs when
the heart is working harder than usual.
- There is a regular pattern to stable angina. After several episodes, you
learn to recognize the pattern and can predict when it will occur. - The pain usually goes away in a few minutes after you rest or take your
angina medicine. - Stable angina is not a heart attack but makes it more likely that you will
have a heart attack in the future. - Unstable angina. Unstable angina is a very dangerous condition that
requires emergency treatment. It is a sign that a heart attack could occur soon.
Unlike stable angina, it does not follow a pattern. It can occur without
physical exertion and is not relieved by rest or medicine. - Variant angina. Variant angina is rare. It usually occurs at rest.
The pain can be severe and usually occurs between midnight and early morning. It
is relieved by medicine.
Not all chest pain or discomfort is angina. Chest pain or discomfort can be
caused by a heart attack, lung problems (such as an infection or a blood clot),
heartburn, or a panic attack. However, all chest pain should be checked
by a doctor.
Other Names for Angina
- Angina pectoris
- Stable or common angina
- Unstable angina
- Variant angina
- Prinzmetal’s angina
- Coronary artery spasms
- Acute coronary syndrome
What Causes Angina?
Angina is caused by reduced blood flow to an area of the heart. This is most
often due to coronary artery disease (CAD). Sometimes, other types of heart
disease or uncontrolled high blood pressure can cause angina.
In CAD, the coronary arteries that carry oxygen-rich blood to the heart
muscle are narrowed due to the buildup of fatty deposits called plaque. This is
called atherosclerosis. Some plaque is hard and stable and leads to narrowed and
hardened arteries. Other plaque is soft and is more likely to break open and
cause blood clots. The buildup of plaque on the inner walls of the arteries can
cause angina in two ways:
- By narrowing the artery to the point where the flow of blood is greatly
reduced - By forming blood clots that partially or totally block the artery
 Stable Angina
Stable Angina
Physical exertion is the most common cause of pain and discomfort from stable
angina. Severely narrowed arteries may allow enough blood to reach the heart
when the demand for oxygen is low (such as when you are sitting). But with
exertion, like walking up a hill or climbing stairs, the heart works harder and
needs more oxygen. Other causes include:
- Emotional stress
- Exposure to very hot or cold temperature
- Heavy meals
- Smoking
Unstable Angina
Unstable angina is caused by blood clots that partially or totally block an
artery. If plaque in an artery ruptures or breaks open, blood clots may form.
This creates a larger blockage. The clot may grow large enough to completely
block the artery and cause a heart attack. Blood clots may form, partly
dissolve, and later form again. Chest pain can occur each time a clot blocks an
artery.
Variant Angina
Variant angina is caused by a spasm in a coronary artery. The spasm causes
the walls of the artery to tighten. This narrows the artery, causing the blood
flow to the heart to slow or stop. Variant angina may occur in people with and
without CAD. Other causes of spasms in the arteries that supply the heart with
blood are:
- Exposure to cold
- Emotional stress
- Medications (vasoconstricting) that constrict or narrow blood vessels
- Cigarette smoking
- Cocaine use
Who Is At Risk for Angina?
More than 6 million people in the United States have angina.
People with coronary artery disease or who have had a heart attack are more
likely to have angina.
Unstable angina occurs more often in older adults.
Variant angina is rare. It accounts for only about 2 out of 100 cases of
angina. People with variant angina are often younger than those with other forms
of angina.
What Are the Signs and Symptoms of Angina?
Pain and discomfort are the main symptoms of angina. These symptoms
- Are often described as pressure, squeezing, burning, or tightness in the
chest - Usually start in the chest behind the breastbone
- May also occur in the arms, shoulders, neck, jaw, throat, or back
- May feel like indigestion
Some people say that angina discomfort is hard to describe or that they can’t
tell exactly where the pain is coming from. Symptoms such as nausea, fatigue,
shortness of breath, sweating, light-headedness, or weakness may also occur.
Symptoms vary based on the type of angina.
Stable Angina
The pain or discomfort:
- Occurs when the heart must work harder, usually during physical exertion
- Is expected, and episodes of pain tend to be alike
- Usually lasts a short time (5 minutes or less)
- Is relieved by rest or angina medicine
- May feel like gas or indigestion
- May feel like chest pain that spreads to the arms, back, or other areas
Unstable Angina
The pain or discomfort:
- Often occurs at rest, while sleeping at night, or with little physical
exertion - Is unexpected
- Is more severe and lasts longer (as long as 30 minutes) than episodes of
stable angina - Is usually not relieved with rest or angina medicine
- May get continuously worse
- May signal that a heart attack will happen soon
Variant Angina
The pain or discomfort:
- Usually occurs at rest and during the night or early morning hours
- Tends to be severe
- Is relieved by angina medicine
Chest pain that lasts longer than a few minutes and is not relieved by rest
or angina medicine may mean you are having—or are about to have—a heart
attack. Call 9–1–1 right away.
How Is Angina Diagnosed?
To find out if you have angina, your doctor will:
- Do a physical exam
- Ask about your symptoms
- Ask about your risk factors and your family history of coronary artery
disease (CAD) or other heart disease
Sometimes, your doctor can diagnose angina by noting your symptoms and how
they occur. Your doctor may order one or more tests to help make a diagnosis of
angina. The tests your doctor may order include:
- EKG or ECG (electrocardiogram). This test measures the rate and regularity
of your heartbeat. Some people with angina have a normal EKG. - Exercise stress test. This test sh