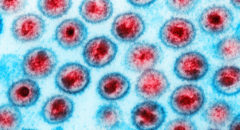
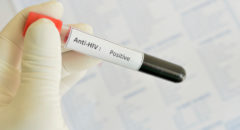
With one in 50 Black Americans infected with HIV–and experts estimating that one in 16 Black men and one in 30 Black women will become infected during their lifetimes–you’d think that folks would use condoms all the time. Yet rising HIV and other STD rates among Black Americans suggest that people are still not using condoms consistently.
With one in 50 Black Americans infected with HIV–and experts estimating that one in 16 Black men and one in 30 Black women will become infected during their lifetimes–you’d think that folks would use condoms all the time. Yet rising HIV and other STD rates among Black Americans suggest that people are still not using condoms consistently.
We found three single men willing to divulge a recent situation in which they snubbed the rubbers. (Names have been changed to protect the identities of the not so innocent, and in a companion article we talked to several condom-averse women.) Then we asked psychologist and sex therapist Gail Wyatt, Ph.D., associate director of the UCLA AIDS Institute, to comment on each situation, offering what we hope will be health- and lifesaving advice.
Riley, Age 35
I didn’t use a condom with one girl because I knew her. We were heavy into foreplay and asked each other if either had condoms and then, “Are you safe?” After sex, she asked me why we didn’t use anything, as if trying to relieve herself of responsibility. She said the guy should always have one in his wallet. So our pillow talk turned into, “When was the last time you got checked? Who were you with last?” It became very clinical. I had plenty of regrets and dark thoughts. I was too reckless. But I got tested, and I’m OK.
SIGN UP FOR OUR NEWSLETTER HERE!
Dr. Wyatt suggests: Many people are confused about how sexually transmitted diseases are transmitted, including HIV. They mistakenly believe that knowing someone, thinking a person looks good or healthy, or is a certain type of person will protect them from becoming infected. But these factors have nothing to do with STDs, which are not transmitted by looks but by bodily fluids. Many nice, loving, good-looking and well-intended people don’t know they’re infected, or are afraid to tell their partners. And once you have an STD, it’s easier to become infected with HIV.
Even when we know our sex partners, we need to remember that they have a past. Our partners’ partners also have pasts, and their partners’ partners have pasts–and so on. Whether you ever see or even know about these other folks, their sexual exposures and risk taking increase your risk exponentially. That’s why it’s essential to wear condoms whenever you are not certain of a person’s status, even if you know him or her. By “certain,” I mean that you’ve seen recent HIV- and other STD-test results on a lab-certified piece of paper and have no doubts that the person is monogamous. If you’re not positive about both, use condoms all the time and get tested regularly so you don’t end up with a disease you can’t get rid of–especially HIV/AIDS.
Jay, Age 41
I was recently with a young lady I’d been dealing with off and on for some time. We got caught up in the moment and didn’t use any protection. I wasn’t too concerned about disease, even though I should have been. She did ask me about my recent partners and sexual behavior. After we had sex, I became uncomfortable because I started thinking about STDs and pregnancy. I have been caught out there on more than one occasion in recent years. I think both men and women should insist that condoms be used. I know I will from now on.
Dr. Wyatt suggests: Before either partner becomes aroused, it’s important to ask, “What kinds of protection do we need to use to prevent STDs, pregnancy and HIV?” In the heat of the moment, people forget that they may be exposing themselves to a lifetime of repercussions. Take control of your sex life and its consequences. If you don’t have condoms now, plan to meet up later–prepared.
Darren, Age 32
Me and my ex-girlfriend had an explosive argument and did not speak for six weeks. She called me one day and ordered me to come get some things I left behind. When I got to her place, I grabbed her and went to work. When we finished, she asked why I did not use anything. I was scared because we had not seen each other for a long time and I had no idea what she had been doing. I ended up getting tested for my job, and thank God, I’m negative. Now I always strap up.
Dr. Wyatt suggests:This dynamic happens even in marriages. People break up, get horny and then go back to their ex for a “touch-up” because that’s the sex partner they know. Then they head out into the world and do whatever with whomever. But whether you are “sex buddies,” “friends with benefits” or cheating, having sex with more than one person dramatically increases your risk of becoming infected. If you go back to your ex to have sex, be sure to ask whether he or she has had other partners. If there is any chance that either of you has slept with other people, use condoms conscientiously and get tested regularly.
Dr. Wyatt’s Wrap-Up
Sexual attraction and arousal are very powerful. All three of these men endangered themselves, even though their reactions afterward show that they knew better. Thankfully, all appear to have avoided getting HIV. What we don’t know is if they have other STDs. Since none of them mentions it, I assume they weren’t tested. They may be infecting other women without knowing it.
Visit the BlackDoctor.org HIV Learning Center for more articles.