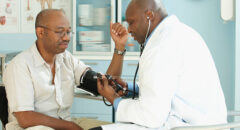
Cancer affects people of all racial and ethnic groups. An estimated 556,500 Americans are expected to die of the disease in 2003.
However, a close look at cancer rates for racial and ethnic groups reveals some significant differences. Such differences have been described as health disparities. A National Institutes of Health working group defined health disparities as differences in the incidence, prevalence, mortality, and burden of cancer and related adverse health conditions that exist among specific population groups in the United States. These population groups may be characterized by gender, age, ethnicity, education, income, social class, disability, geographic location, sexual orientation.
One important example of a health disparity is African-Americans higher overall cancer incidence and mortality (death) rates compared to other groups. Additionally, certain racial/ethnic groups experience higher rates for specific cancers than other groups.
Many of the differences in cancer incidence and mortality rates among racial and ethnic groups may be due to factors associated with social class rather than ethnicity. Socioeconomic status (SES) in particular appears to play a major role in the differences in cancer incidence and mortality rates, risk factors, and screening prevalence among racial and ethnic minorities. Moreover, studies have found that SES, more than race, predicts the likelihood of a groups access to education, certain occupations, and health insurance, as well as income level and living conditions, all of which are associated with a persons chance of developing and surviving cancer.
One purpose of this fact sheet is to give a brief overview of the currently available data on cancer health disparities among racial and ethnic groups. The rates are based on statistics from the National Cancer Institute (NCI) and the National Center for Health Statistics.* It should be noted that these agencies are concerned that the small size of some non-white population groups and the methods used to collect data have the potential to yield counts that are unrepresentative of the group as a whole. Work to overcome these problems is ongoing (see under Selected NCI Research Activities, SEER Program Expansion).
The fact sheet also summarizes some NCI research projects and initiatives designed to understand and eventually eliminate these disparities.
CANCER RATES
OVERALL INCIDENCE AND MORTALITY RATES. The following U.S. incidence and death rates are for all cancers combined.
• Cancer Incidence Rates (Number of new cases each year).
Statistics are for 1996-2000, are adjusted to the 2000 U.S. standard million population, and represent the number of new cases of invasive cancer per year per 100,000 of both sexes, males, and females, respectively.
| Group | Both Sexes | Males | Females |
| African-American | 521.7 | 696.8 | 406.3 |
| White | 479.8 | 555.9 | 431.8 |
| Asian/Pacific Islande | 341.7 | 392.0 | 306.9 |
| Hispanic/Latino | 352.1 | 419.3 | 312.2 |
| Amer Ind/Alaska Nat | 239.6 | 259.0 | 229.2 |
• Cancer Death Rates (Number of deaths each year).
Statistics are for 1996-2000, are adjusted to the 2000 U.S. standard million population, and represent the number of deaths per year per 100,000 of both sexes, males, and females, respectively.
| Group | Both Sexes | Males | Females |
| African-American | 257.1 | 356.2 | 198.6 |
| White | 199.1 | 249.5 | 166.9 |
| Asian/Pacific Islander | 124.5 | 154.8 | 102.0 |
| Hispanic/Latino | 137.9 | 176.7 | 112.4 |
| Amer Ind/Alaska Nat | 138.0 | 172.3 | 115.8 |
AFRICAN-AMERICANS
African-Americans have the highest incidence and death rates overall, as well as the highest rates for certain cancers.
• African-American Females: Highest incidence rates for certain cancers.
Among females, African-Americans have the highest incidence rates of certain cancers, such as colon and rectal cancer and lung and bronchus cancer. Rates are also available for whites, Asian/Pacific Islanders, Hispanics/Latinas, and American Indian/Alaska Natives for these and other cancer sites. Statistics are for 1996-2000, are adjusted to the 2000 U.S. standard million population, and represent the number of new cases of invasive cancer per year per 100,000 females.
| Group | Colon and Rectum–Female Incidence | Lung and Bronchus–Female Incidence |