The COVID-19 pandemic’s impact has been felt in communities across the U.S., from the largest urban centers to the smallest rural communities. Black Americans (8.2 percent) are the second-largest minority group, behind Hispanics, in rural and small-town areas.
Prior research has demonstrated, rural communities face unique challenges in responding to the pandemic due to inequities in the medical workforce and provision shortages, including higher medical risks and limited telehealth access.
Non-metro and rural counties experienced an elevated rate of growth in the spread of the virus. Countless stories of the most rural communities being impacted by the coronavirus include remote areas in Alaska and ranches in Texas.
Pew Research Center found that twice the number of coronavirus-related deaths existed in sparsely populated rural areas than in urban areas.
There is cause for concern because research finds that rural residents are among the most vaccine-hesitant groups, along with Republicans, individuals 30-49 years old, and Black adults.
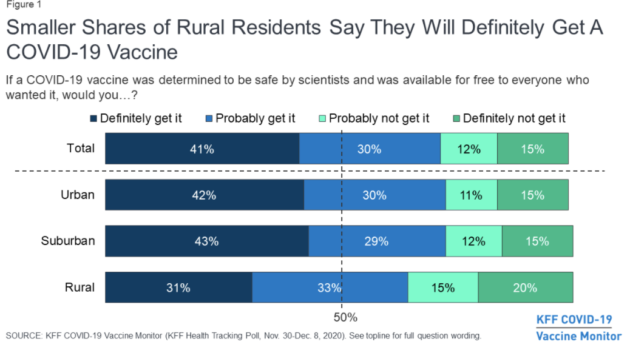
Individuals living in rural areas in the U.S. are significantly less likely to say they will get a COVID-19 vaccine that is deemed safe and available for free than individuals living in suburban and urban America. Slightly less than one-third (31%) of the people in rural areas say they will “definitely get” the vaccine, compared four in ten people in urban areas (42%) and suburban areas (43%).
An additional one-third of people in rural areas say they will “probably get it” while 35% say they will either “probably not get it” (15%) or “definitely not get it” (20%).
Factors associated with one’s willingness to get the coronavirus vaccine include their age, level of education, and – notably – their political party identification. For example, the KFF COVID-19 Vaccine Monitor finds that








