Bola Sogade:
Good afternoon. Heart disease is still the leading cause of death for both men and women and it disproportionately affects African-American women and men. Heart disease claims more than six hundred and thirty-five thousand two hundred and sixty (635,260) American lives in 2016. This means that one in every four United States individuals died of heart disease in 2016.
I have seen firsthand the profound and lasting effects of access to all aspects of a good cardiovascular health and I have also seen the devastating effects of a lack of access. This experience is the foundation of my comments today.
Nakela Cook:
I wanted to tell you a little bit about the nation’s long-term investments in biomedical research which have just contributed to one of the greatest success stories that we have, and it’s really about the fact that over 70 percent decrease in death rates due to heart disease have occurred since the late 1950s. But despite this progress, we know that there’s so much more that needs to be done. Since 2011, the declines in these death rates have started to slow and level off and we’re seeing the prevalence of such diseases like diabetes and obesity at increasingly alarming rates.
We must continue to look at the innovative ways that we can use research to help reach individuals and families and support the necessary lifestyle changes that can really be transformative for our health. And today, we have individuals who agreed to share their own stories and we’re so grateful to have them here with us.
George A. Mensah:
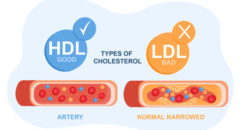
All the research evidence we have suggests that the major risk factors for heart attack and heart disease are the same in women as they are in men. They are just as important in women as they are in men. And in fact, they ought to be treated as seriously in women as they are in men. Forget the pregnancy-related…, I mean, we can’t forget about it, but the real issue is: we’re talking about long-standing high blood pressure that is not controlled, long-standing high cholesterol that is not controlled, long-standing high blood sugar or diabetes that is not controlled, tobacco use, a high body mass index, there’s about seven of these that collectively really increase your risk after carcasses
Ileana L. Pina:
All the doctor knew you belong to me, don’t let anybody change anything especially my heart favor vessel, don’t let anybody change anything because it’s your mind, and if they try to change it, you call me first. So that sense of ownership especially for the Hispanics but also for the African-Americans is really really critical because now there’s a bond, they know that there’s one individual who really cares about what they’re doing, I’ll yell at them and I’ll put my finger at them, and they know that it’s because I love them, and I’ll hug them, to know that I love them and I want them to get better, so that connection has been missing.
Michelle N. Johnson:
About 40 percent of African-American patients have hypertension, 50 percent of Hispanic patients have 3:30-3:35[INAUDIBLE] which makes it even more challenging to treat patients, 3:39-3:42[INAUDIBLE], afterwards, we have more aggressive hypertension, and we have more 3:47-3:56[INAUDIBLE], complications, and then makes this type of discussions really critical.
Natalia Rogers:
But Latina women as well as African-American women, we tend to be the caregivers, we tend to play ourselves to the side and say you know what we’ll take care of that, we tend to ignore whatever little wants is going on [inaudible], and say oh we’ll get to that later. We have to start paying attention, I know that I come from a background where my mom, she had a heart attack that contributed to her death that was in conjunction with cancer, my Father had a cardiac arrest, the procedures failed, and my grandfather; my paternal grandfather, he also died in his sleep from stroke.
Sharon Bond:
At age 47, I had a Heart Attack, it went 47 years undetected, so this is something that’s really important and I believe that the researchers, doctors and all. I am someone who goes to the gym, go to the doctor, all my physicals, everything, and for 47 years nothing, no one saw anything and I don’t know if they didn’t see it because they didn’t want to see it or they’ve heard it and didn’t want to mention it, I’m not really sure. But that connection from the doctor to the patient, for me It’s so so important. We mentioned American Heart Association, I jumped right on the internet as soon as I found out that I had Hypotrpiccardiomyopathy, a long word never heard of it before, didn’t know what it was.
Soon as I typed it in, and I typed it in as it sounds, then but it came up, American Heart Association came up and I’m looking and I’m going through and I say you know what, I need to get involved because what I want to do is I want to let other women and men, kids, whoever’s listening know, what I went through if it can be prevented, let it be prevented.
Let us all take away one thing from this that’ll really help us change the lives of our families, our patients, and our community. So thank you so much for all and each of you. [Applause]