It’s rare in the human body that events happen in a vacuum—and very much like “The Skeleton” song suggests—everything is connected. And beyond the skeleton, the saying is especially true within the cardiovascular system. Known as the “king of systems,” the cardiovascular system is a complex network of veins and arteries that impact every part of the human body.
It’s rare in the human body that events happen in a vacuum—and very much like “The Skeleton” song suggests—everything is connected. And beyond the skeleton, the saying is especially true within the cardiovascular system. Known as the “king of systems,” the cardiovascular system is a complex network of veins and arteries that impact every part of the human body.
So it only makes sense that there is a relationship between cholesterol and hypertension (or high blood pressure). According to the Centers for Disease Control and Prevention, 29 percent of Americans—roughly 70 million people—suffer from hypertension, and studies suggest that those with high cholesterol are more likely to develop hypertension. The numbers are even higher for African Americans—more than 40 percent are living with high blood pressure.
Men with an elevated risk for atherosclerosis (‘hardening of the arteries’) are also vulnerable to metabolic syndrome, a condition that increases your risk for coronary heart disease and stroke. Other risk factors, like a high LDL (bad) cholesterol level and smoking, are contributors for heart and other vascular diseases.
I refer to the definition of metabolic syndrome utilized by the National Heart, Lung and Blood Institute as follows:
* Excess fat in the stomach area is a greater risk factor for heart disease than excess fat in other parts of the body, such as on the hips.
* A high triglyceridelevel. Triglycerides are a type of fat found in the blood.
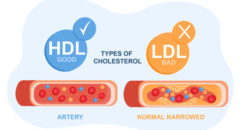
* A low HDL (good) cholesterol level
* High blood pressure.
* High fasting blood sugar. Mildly high blood sugar may be an early sign of diabetes.
People at greatest risk for metabolic syndrome have these underlying causes:
- Abdominal obesity (a large waistline
- An inactive lifestyle
- Insulin resistance (which can lead to type 2 diabetes and prediabetes because the beta cells fail to keep up with the body’s increased need for insulin; excess glucose then builds up in the bloodstream, leading to diabetes, prediabetes, and other serious health disorders
- In clinical practice, risk factors (traits, conditions, or habits that increase your chance of developing a disease) can be addressed as follows:
- Modifiable risk factors can be addressed with weight optimization, regular aerobic exercise, lean eating, using healthy oils vs. saturated fat intake, BP/blood glucose/triglyceride control and optimization of HDL levels (the ‘good’ cholesterol).
- Risk factors you cannot control are increasing age and genetic predisposition (i.e. ethnicity, family history)
At risk men should be particularly vigilant in monitoring their condition with a physician. Some men respond particularly well to a shared-decision-making style of primary medical care, partnering with a trusted clinician to not only diagnose these conditions and to identify risk factors but also to help to ‘coach’ them to successful lifestyle changes and medical management adherence. Such ‘patient engagement’ (also leveraging online and social networking tools) can help to reduce the risk of adverse outcomes such as heart attack, stroke and other vascular/occlusive diseases as well as other complications of small and large vessel occlusive vascular disease.
So, controlling your cholesterol and blood pressure aren’t mutually exclusive. According to the American Heart Association, cholesterol and lipid abnormalities are one of the major controllable risk factors for coronary heart and other vascular diseases with rising blood cholesterol and various dyslipidemias consistently linked to hypertension (high blood pressure). While both conditions are major risk factors in contributing to heart disease and other diseases of the vascular system, it is important to remember that for most men a healthy lifestyle of optimal cardiovascular fitness and heart-healthy eating can go a long way toward maintaining one’s health and longevity.
Dr. Gregory Pecchia is a member of the Board of Advisors with Men’s Health Network and a practicing physician based in La Quinta, CA.
# # #