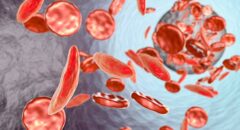
carrying oxygen through the blood and into tissues such as muscles and organs. The lack of hemoglobin causes the cells to be malformed and brittle, which leads to a disruption in the normal blood flow through vessels and arteries. When blood is pumped from the heart and travels through arteries to distal parts of the body vessels become smaller.
The narrowing of these vessels can cause sickled red blood cells to become clogged and coagulated at various junctions, leading to extreme pain. In addition to the cells becoming clogged in arteries, the immature red blood cells are also fragile leading to rupture. The pain is commonly felt in the muscles and bones and has been described as throbbing, stabbing, dull or sharp pains.
In sickle cell anemia there are three primary mechanisms of pain arousal; nociceptive, peripheral neuropathic and central neuropathic pain. Inflammation or mechanical tissue pain is the underlying cause of nociceptive pain and is generally characterized by local throbbing, sharp and pounding pain.
Nociceptive pain tends to respond favorably to NSAIDs and opioid medications. Damaged or dysfunctional peripheral nerves can cause neuropathic pain commonly described as burning, heaviness, and numbness.
Patients suffering from peripheral neuropathy respond positively to pharmacological therapies. Damage to central nerves in the spine and brain can result in altered pain processing, causing normal stimuli to trigger intense pain responses. Central neuropathies respond favorably to neuroactive medications that alter the levels of pain neurotransmitters released.
Symptoms of sickle cell anemia have been noted to have