Hemodialysis is the most common method used to treat advanced and permanent
Hemodialysis is the most common method used to treat advanced and permanent
kidney failure. Since the 1960s, when hemodialysis first became a practical
treatment for kidney failure, we’ve learned much about how to make hemodialysis
treatments more effective and minimize side effects. But even with better
procedures and equipment, hemodialysis is still a complicated and inconvenient
therapy that requires a coordinated effort from your whole health care team,
including your nephrologist, dialysis nurse, dialysis technician, dietitian, and
social worker. But the most important members of your health care team are you
and your family. By learning about your treatment, you can work with your health
care team to give yourself the best possible results, and you can lead a full,
active life.
When Your Kidneys Fail
Healthy kidneys clean your blood by removing excess fluid, minerals, and
wastes. They also make hormones that keep your bones strong and your blood
healthy. When your kidneys fail, harmful wastes build up in your body, your
blood pressure may rise, and your body may retain excess fluid and not make
enough red blood cells. When this happens, you need treatment to replace the
work of your failed kidneys.
How Hemodialysis Works
In hemodialysis, your blood is allowed to flow, a few ounces at a time,
through a machine with a special filter that removes wastes and extra fluids.
The clean blood is then returned to your body. Removing the harmful wastes and
extra salt and fluids helps control your blood pressure and keep the proper
balance of chemicals like potassium and sodium in your body.
One of the biggest adjustments you must make when you start hemodialysis
treatments is following a rigid schedule. Most patients go to a clinic—a
dialysis center—three times a week for 3 to 5 or more hours each visit. For
example, you may be on a Monday-Wednesday-Friday schedule or a
Tuesday-Thursday-Saturday schedule. You may be asked to choose a morning,
afternoon, or evening shift, depending on availability and capacity at the
dialysis unit. Your dialysis center will explain your options for scheduling
regular treatments.
A few centers teach people how to perform their own hemodialysis treatments
at home. A family member or friend who will be your helper must also take the
training, which usually takes at least 4 to 6 weeks. Home dialysis gives you a
little more flexibility in your dialysis schedule, but a regular schedule is
still important. With home hemodialysis, the time for each session and the
number of sessions per week may vary.

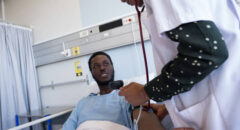
Hemodialysis.
Adjusting to Changes
Even in the best situations, adjusting to the effects of kidney failure and
the time you spend on dialysis can be difficult. Aside from the “lost time,” you
may have less energy. You may need to make changes in your work or home life,
giving up some activities and responsibilities. Keeping the same schedule you
kept when your kidneys were working can be very difficult now that your kidneys
have failed. Accepting this new reality can be very hard on you and your family.
A counselor or social worker can help you cope.
Many patients feel depressed when starting dialysis, or after several months
of treatment. If you feel depressed, you should talk with your social worker,
nurse, or doctor because this is a common problem that can often be treated
effectively.
 Arteriovenous fistula. |
Getting Your Vascular Access Ready
One important step before starting hemodialysis is preparing a vascular
access, a site on your body from which your blood is removed and returned. A
vascular access should be prepared weeks or months before you start dialysis. It
will allow easier and more efficient removal and replacement of your blood with
fewer complications. For more information about the different kinds of vascular
accesses and how to care for them, see the National Institute of Diabetes and
Digestive and Kidney Diseases (NIDDK) fact sheet Vascular Access for
Hemodialysis.

Graft.
Equipment and Procedures
When you first visit a hemodialysis center, it may seem like a complicated
mix of machines and people. But once you learn how the procedure works and
become familiar with the equipment, you’ll be more comfortable.
Dialysis Machine
The dialysis machine is about the size of a large television. This machine
has three main jobs:
- pump blood and monitor flow for safety
- clean wastes from blood
- monitor your blood pressure and the rate of fluid removal from your
body
 Structure of a typical hollow Structure of a typical hollowfiber dialyzer. |
Dialyzer
The dialyzer is a large canister containing thousands of small fibers through
which your blood is passed. Dialysis solution, the cleansing fluid, is pumped
around these fibers. The fibers allow wastes and extra fluids to pass from your
blood into the solution, which carries them away. The dialyzer is sometimes
called an artificial kidney.
- Reuse. Your dialysis center may use the same dialyzer more than once
for your treatments. Reuse is considered safe as long as the dialyzer is cleaned
and disinfected before each use. The dialyzer is tested each time to make sure
it’s still working, and it should never be used for anyone but you. Before each
session, you should be sure that the dialyzer is labeled with your name and
check to see that it has been cleaned, disinfected, and tested.
Dialysis Solution
Dialysis solution, also known as dialysate, is the fluid in the dialyzer that
helps remove wastes and extra fluid from your blood. It contains chemicals that
make it act like a sponge. Your doctor will prescribe a specific dialysate for
your treatments. This formula can be adjusted based on how well you tolerate the
treatments and on your blood tests.
Needles
Many people find the needle sticks to be one of the most unpleasant parts of
hemodialysis treatments. Most people, however, report getting used to them after
a few sessions. If you find the needle insertion painful, an anesthetic cream or
spray can be applied to the skin.
Most dialysis centers use two needles—one to carry blood to the dialyzer and
one to return the cleaned blood to your body. Some specialized needles are
designed with two openings for two-way flow of blood, but these needles are less
efficient and require longer sessions. Needles for high-flux or high-efficiency
dialysis need to be a little larger than those used with regular dialyzers.

Arterial and venous
needles.
Some people prefer to insert their own needles. You’ll need ins