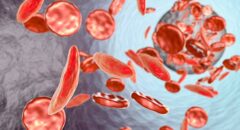
red blood cell than an older child. Even newborns with the sickle cell gene make healthy blood cells, thanks to fetal hemoglobin, which allows a fetus to get enough oxygen from its mother’s blood. But the body usually stops making it a few months after birth.
About 12 years ago, researchers at the center identified the gene that controls the manufacturing of fetal hemoglobin, called BCL11A. If they could just keep this gene from shutting off production of fetal hemoglobin, they reasoned, they could prevent most or all of the symptoms of sickle cell.
However, the caveat was figuring out how to make the genetic fix to every red blood cell, and not to other cells where it might cause side effects. Luckily through years of experimentation, the researchers learned how to infect the right cells with a virus that inserts the genetic fix. Once the cells are edited, they can be infused back into the body of a patient whose own red blood cells have been killed with chemotherapy.
Then, they should start making enough fetal hemoglobin to prevent problems from sickle cell.
Despite promising results, it’s unclear if the effects of treatment will last and it’s likely to be at least three years before a genetic therapy for sickle cell disease is approved.
“We are in uncharted territory,” Dr. David A. Williams, chief scientific officer at