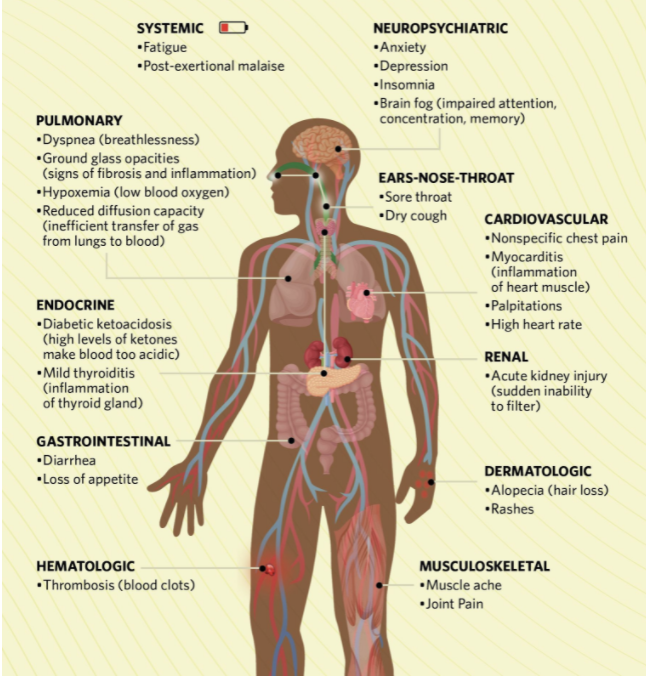
A systematic review of 57 studies involving more than 250,000 COVID-19 survivors reveals that 54% still had at least one symptom 6 months or more after initial diagnosis or release from the hospital.
In the review, published today in JAMA Network Open, a team led by Hershey (Pennsylvania) Medical Center researchers searched the literature from December 2019 through March 2021 for studies on persistent COVID-19–related symptoms diagnosed using lab results, radiologic findings, or clinical signs or symptoms at or after 1 month.
62% had chest imaging abnormalities
At 1 month (short term), a median of 54% of patients (13 studies) reported at least one long COVID-19 symptom, as did 55% (38) at 2 to 5 months (intermediate term), and 54% (9) at 6 months or more (long term).
The most common symptoms of mental, lung, and neurologic disorders; functional mobility problems; and general and constitutional issues were abnormalities on chest imaging (median, 62.2%; 4 studies), trouble concentrating (23.8%; 4), generalized anxiety disorder (29.6%; 7), general functional impairments (44.0%; 9), and fatigue or muscle weakness (37.5%; 30).
In addition to difficulty concentrating, neurocognitive symptoms included memory problems (median, 18.6%; 4 studies), cognitive impairment (17.1%; 7), loss of taste (11.2%; 18), and loss of smell (13.4%; 24).
Mental illness, in addition to generalized anxiety disorder, included sleep disorders (median, 27.0%; 10 studies), depression (20.4%; 2), and posttraumatic stress disorder (13.3%; 9). Lung symptoms included shortness of breath (median, 29.7%; 38 studies) and cough (13.1%; 26). Nearly two thirds (median, 65.0%; 3 studies) needed extra oxygen. Among functional mobility impairments, mobility decline was reported by a median of 20.2% (6 studies) and lower exercise tolerance by a median of 14.7% (2).
The most common general and constitutional symptoms included joint pain (median, 10.0%; 11 studies) and flu-like symptoms (10.3%; 6). Other such symptoms included general pain (median, 32.4%; 8 studies), fever (0.9%; 16), and muscle pain (12.7%; 13). Cardiac symptoms included chest pain (median, 13.3%; 14 studies) and palpitations (9.3%; 5). Heart attack and heart failure were uncommon.
Gastrointestinal symptoms such as abdominal pain, decreased appetite, diarrhea, and vomiting occurred in 6% of COVID-19 survivors. Hair loss was reported by a median of 20.8% of patients (4 studies), as were skin rash (2.8%; 3) and sore throat (3.3%; 6).
Mean patient age was 54.4 years, 56% were male, and 79% were hospitalized during their initial illness. Forty-five studies (79%) came from high-income countries.
‘One-stop’ multidisciplinary clinics needed
After stratification by World Bank income group, median long COVID-19 symptoms were reported by 54.6% (45 studies) in high-income countries and 56.0% (12) in low- and middle-income countries. Symptom rates were comparable in studies with higher (60% or higher) and lower proportions of hospitalized patients.
“These long-term PASC [post acute sequelae of COVID-19] effects occur on a scale that could overwhelm existing health care capacity, particularly in low- and middle-income countries,” the authors wrote.
Treatment of long COVID-19 symptoms, the authors said, requires a whole-patient perspective, including virtual rehabilitation platforms and long-term treatment of these symptoms as well as pre existing or new underlying conditions.
“One-stop multidisciplinary clinics are therefore recommended to avoid multiple referrals to different specialists and encourage comprehensive care,” the researchers wrote.
“These specialists should include respiratory physicians, cardiologists, neurologists, general physicians (from primary care or rehabilitation medicine), neuropsychologists or neuropsychiatrists, physiotherapists, occupational therapists, speech and language therapists, and dieticians [sic].”








