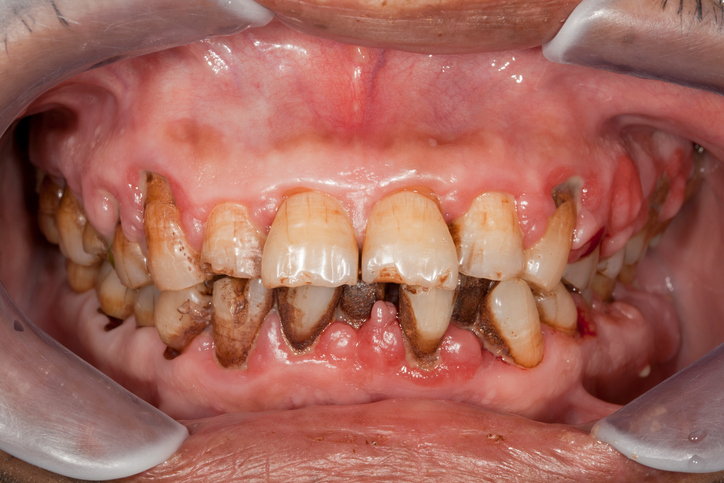
If you have been told you have periodontal (gum) disease, you’re not alone. An estimated 80 percent of American adults currently have some form of the disease.
Periodontal diseases range from simple gum inflammation to serious disease that results in major damage to the soft tissue and bone that support the teeth. In the worst cases, teeth are lost.
A new study from the Centers for Disease Control and Prevention (CDC) confirms that nearly one out of two U.S. adults age 30 and over—have periodontitis, the advanced form of periodontal disease. The findings, reported in the Journal of Periodontology, also indicate that prevalence is highest among ethnic minorities, with 63.5 percent of Hispanic-Americans, 59.1 percent of African Americans and 50 percent of Non-Hispanic Asian Americans affected by periodontitis.
Gum disease is not just a threat to your mouth and oral health, it’s a threat to your overall health. Research is also pointing to possible health effects of periodontal diseases that go well beyond your mouth (more about this later). Whether it is stopped, slowed, or gets worse depends a great deal on how well you care for your teeth and gums every day, from this point forward.
What causes periodontal disease?
Our mouths are full of bacteria. These bacteria, along with mucus and other particles, constantly form a sticky, colorless “plaque” on teeth. Brushing and flossing help get rid of plaque. Plaque that is not removed can harden and form bacteria-harboring “tartar” that brushing doesn’t clean. Only a professional cleaning by a dentist or dental hygienist can remove tartar.
Gingivitis
The longer plaque and tartar are on teeth, the more harmful they become. The bacteria cause inflammation of the gums that is called “gingivitis.” In gingivitis, the gums become red, swollen and can bleed easily. Gingivitis is a mild form of gum disease that can usually be reversed with daily brushing and flossing, and regular cleaning by a dentist or dental hygienist. This form of gum disease does not include any loss of bone and tissue that hold teeth in place.
Periodontitis
When gingivitis is not treated, it can advance to “periodontitis” (which means “inflammation around the tooth.”) In periodontitis, gums pull away from the teeth and form “pockets” that are infected. The body’s immune system fights the bacteria as the plaque spreads and grows below the gum line. Bacterial toxins and the body’s enzymes fighting the infection actually start to break down the bone and connective tissue that hold teeth in place. If not treated, the bones, gums, and connective tissue that support the teeth are destroyed. The teeth may eventually become loose and have to be removed.







