Public health officials are closely tracking a new superbug. It’s a surprisingly new strain of fungus called Candida auris, and it’s resistant to most of the drugs that are available to treat it.
Studies estimate that about half of people who become infected with it will die. According to the latest update from the CDC, it has sickened 617 patients in hospitals, nursing homes, and long term care facilities in 12 states.
Candida auris was first discovered in 2016. The first cases appeared after a short while when the signs of infection were spotted in the US. According to official statistics provided by the CDC, the number of cases recorded in the US has reached 617, with most of them being located in areas like New York, Chicago, and New Jersey.
The spread of the fungus has been encouraged by a variety of factors. In comparison to other species of Candida, this particular fungus is more prone to transmission from person to person. It is also more resistant on surfaces, and it can survive routine cleaning procedures, making hospitals and other medical environments an ideal ground for further spread.
A well-known researcher has stated that medical centers need to change their cleaning strategy if they wish to mitigate the growing rate of infections.
Another issue is posed by the fact that Candida auris is particularly resilient against most of the antifungal medications which are currently available on the market, a trait which renders it very difficult to treat.
Such a degree of resilience hasn’t been observed in other Candida species, and some researchers think that it may be linked to the current use of antifungal medication.
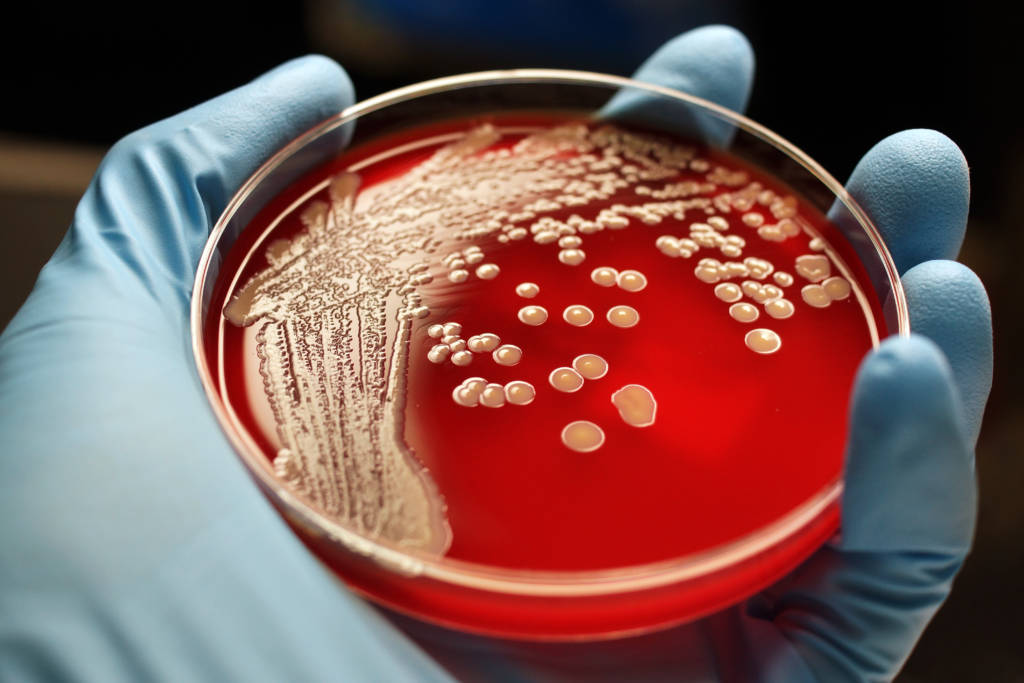
Of 140 patients infected during the first 10 months of a recent outbreak in Spain, 41 developed invasive blood infections. Even with treatment, 17 people died, according to a journal article.
There is also the fact that some lab tests will not identify the superbug as the source of an illness, which means that some patients will receive the wrong treatment, increasing the duration of the infection and the chance to transmit the fungus to another person.
Data from the CDC notes patients who spent a long period in a hospital, use a central venous or catheter or other invasive tubes have a higher risk of contracting the superbug.
Drug-Resistant HIV On The Rise
 The World Health Organization (WHO) warns that resistance to the drugs used to treat HIV is on the rise.
The World Health Organization (WHO) warns that resistance to the drugs used to treat HIV is on the rise.
According to the 2017 WHO HIV Drug Resistance report, 6 out of 11 countries surveyed reported that more than 10 percent of people who are “starting antiretroviral therapy had a strain of HIV that was resistant to some of the most widely used HIV medicines.”
“Antimicrobial drug resistance is a growing challenge to global health and sustainable development,” said Dr. Tedros Adhanom Ghebreyesus, WHO Director-General. “We need to proactively address the rising levels of resistance to HIV drugs if we are to achieve the global target of ending AIDS by 2030.”
More than half a dozen countries are above the 10 percent threshold. These include Argentina, Guatemala, Namibia, Nicaragua, Uganda and Zimbabwe. Researchers warn that the growing threat could undermine global progress in treating and preventing HIV infection if action is not taken immediately.
In 2014, there were an estimated 37,600 new HIV infections, says the Centers for Disease Control and Prevention (CDC). During that time, an estimated 1.1 million people in the United States were living with the fatal disease.
One in 7 (about 15 percent) did not know their status. As of June 2016, about 36.7 million people were living with HIV globally, with 19.5 million receiving medicines to treat the illness, called antiretroviral therapy (ART).
Antiretroviral therapies have helped people live substantially longer with HIV. A study published in the Lancet HIV reported that a 20-year-old infected with HIV today can expect to live about 78 years, which is comparable to individuals who do not have the disease.
Still, the new data proves that a growing number of sufferers are experiencing the consequences of drug resistance. Drug resistance occurs when people don’t adhere to a prescribed treatment plan. This often happens because they don’t have access to high-quality HIV treatment or care and can’t take their full regimen of medication.
"We need to ensure that people who start treatment can stay on effective treatment, to prevent the emergence of HIV drug resistance," said Dr. Gottfried Hirnschall, director of WHO’s HIV Department and Global Hepatitis Program, in statement about the findings. “When levels of HIV drug resistance become high we recommend that countries shift to an alternative first-line therapy for those who are starting treatment.”
Know Your Status
Therein lies the importance of early detecting via testing. Ways to know your status include:
- Ask your primary care physician for an HIV test.
- Test at home with OraQuick, the FDA-approved in-home HIV test.
- Check local substance abuse programs, community health centers and hospitals about free testing events.
- Call 1-800-CDC-INFO (232-4636) for testing locations near you.
- Visit gettested.cdc.gov or locator.hiv.gov for testing locations.
- You can even get updates via text messag, by texting KNOW IT (566948) with your zip code.